Translational Perioperative and Pain Medicine (ISSN: 2330-4871)
ARTICLE DOI: 10.31480/2330-4871/116
Review ArticleOPEN ACCESS
Perioperative Care Provider's Considerations in Managing Patients with the COVID-19 Infections
Xiangdong Chen1, You Shang1, Shanglong Yao1, Renyu Liu2 and Henry Liu3*
1Department of Anesthesiology, Institute of Anesthesia and Critical Care Medicine, Union Hospital of Tongji Medical College, Huazhong University of Science and Technology, 1277 Jiefang Avenue, Wuhan, Hubei 430022, China
2Department of Anesthesiology and Critical Care, Hospital of the University of Pennsylvania, 3400 Spruce Street, Suite 680 Dulles, Philadelphia, PA 19104, USA
3Department of Anesthesiology & Perioperative Medicine, Penn State Milton S. Hershey Medical Center, 500 University Drive, H187, Hershey, PA 17033, USA
Henry Liu, MD, Department of Anesthesiology & Perioperative Medicine, Penn State Milton S. Hershey Medical Center, 500 University Drive, H187, Hershey, PA 17033, USA, Email: henryliupa@gmail.com
Editor: Yuanxiang Tao, MSc, PhD, MD, Professor/Vice Chair of Research, Department of Anesthesiology, New Jersey Medical School, Rutgers, The State University of New Jersey, Newark, NJ 07103, USA, Email: yt211@njms.rutgers.edu
Received: February 11, 2020 | Accepted: February 13, 2020 | Published: February 15, 2020
Citation: Chen X, Shang Y, Yao S, Liu R, Liu H. Perioperative Care Provider's Considerations in Managing Patients with the COVID-19 Infections. Transl Perioper & Pain Med 2020; 7(2):216-224.
Abstract
The COVID-19 (also named as 2019-nCoV) is a very contagious novel coronavirus. Though most patients contracted the 2019-nCoV will likely have mild symptoms with good prognosis, some will develop severe acute respiratory infection, pneumonia, or acute respiratory distress syndrome. Some of these patients will need anesthesia care for endotracheal intubation, critical care management and surgical services. Perioperative care services will face enormous challenges in managing these patients with the COVID-19. The challenges are how to protect perioperative care providers and how to avoid cross-infection by transmitting the COVID-19 to other individuals, in addition to managing their respiratory failure and other pathophysiological disturbances. In this article, we discussed the personal protective equipment and techniques of using them, and strategies to prevent or minimize the probability of cross-infection of the COVID-19 from infected patient to other individuals. Perioperative care provider's self-protection includes universal precautions, wearing gloves, facemask, eye protections, and coverall gowns. Preventive measures of cross-infection include isolation room in paranesthesia holding area or straight to the operating room bypassing paranesthesia holding area, ventilation circuit filter(s), and circuit, CO2 absorbent and cannister replacement after each use, airborne and droplet precautions, and establishment of department and hospital-wide crisis management protocols. Perioperative care providers may encounter numerous unexpected difficulties such as poor visibility inside the coverall gowns, difficult to communicate verbally due to voice baffling, providers may become hyperthermia and sweating inside the gowns. The COVID-19 is a new disease, its transmission, clinical presentation, diagnosis and management are evolving, our perioperative care will need modification accordingly.
Keywords
Novel coronavirus, 2019-nCoV, COVID-19, Airborne precaution, Pneumonia, Acute respiratory distress syndrome
Introduction
In December 2019, a novel coronavirus (2019-nCoV, now named as COVID-19) has emerged and been identified in Wuhan, Hubei province, China. Patients infected by this COVID-19 could develop severe acute respiratory infection and pneumonia, and potentially quickly evolve into acute respiratory failure, acute respiratory distress syndrome (ARDS), and other serious systemic multi-organ failure complications [1,2]. The COVID-19 have been confirmed that it can have transmissions from human-to-human. The COVID-19 is extremely contagious. It can be transmitted through aerosol/aerated solids or fluid from human secretions or discharges, as well as droplets from normal breathing, coughing, sneezing and surface contact [1-3]. These modalities of transmission will pose tremendous risk for the perioperative care providers in the operating room and other perioperative settings. Perioperative care providers may get contracted during caring of these patients, and their infected patients may pass the COVID-19 to other individuals by cross-infection. This article will focus on perioperative care providers' self-protection and avoidance of cross-infection and in-hospital infection.
Self-precaution for Perioperative Care Providers
All perioperative care providers need to well protect themselves during the process of caring for their patients. When taking care of patients with highly contagious disease, it cannot be over emphasized how important it is to protect healthcare providers themselves. Personal protections include two aspects: Wearing protective equipment and applying universal precautions. Personal protective equipment includes eye-protective goggles, face mask, face shield, gloves, and various gowns.
Face mask
a. Commonly used face masks: Masks are categorized based on oil resistance (letter NRP) and how much air particles can be filtered (i.e., 95), based on NIOSH classifications. N means not oil resistant, R stands for oil resistant, and P indicates oil proof. The number 95 means 95% of air particles will be filtered out. The number 100 indicates 99.97% air particles will be filtered out, In Europe, P1 or FFP1 means 80% of air particles will be filtered out, P2, or FFP2, 94%, and P3, or FFP3, 99.95%, as shown in Table 1.
Table 1: Mask Classifications in USA, Europe, and China [4].
| US NIOSH | Europe | China (GBT 32610-2016) | |||||
| Letter | Number | Symbol | Number | Symbol | Detection by Sodium oxide | Detection by oil | |
| N | 95 | P1 | FFP1 | 80 | KN90 KN95 KN100 |
90 95 99.97 |
N/A |
| R | 99 | P2 | FFP2 | 94 | KP90 KP95 KP100 |
N/A | 90 95 99.97 |
| P | 100 | P3 | FFP3 | 99.95 | |||
b. Techniques of wearing a facemask (put on, use, take off and dispose after use) [5], as shown in Figure 1.

Figure 1: Face mask and shield.
1). Before putting on a mask, hands are cleaned with soap and water, or alcohol-based hand rub;
2). Face mask should cover over mouth and nose and make sure there is no gap between face and the mask;
3). Avoid touching the mask while using it, especially after contacting patient;
4). If you by accident touched mask after contacting patient, clean hands with soap and water, or alcohol-based hand rub. Then replace the mask with a new one;
5). Do not re-use single-use face masks;
6). After using face mask, remove it from behind without touching the front of face mask; and discard it immediately into a designated biohazard container; and clean hands with a soap and water, or alcohol-based hand rub [5].
Gloves
1. Types of medical gloves and their Uses (Table 2)
Table 2: Types of medical gloves and their Uses [6].
| Types of gloves | Gloves’ features |
| Latex gloves | • Powdered or powder-free • Flexible • Great fit • Sensitivity to touch • Moderate protection • Can cause allergies and skin irritation |
| Vinyl gloves | • High quality yet cost effective • Made from PVC • Moderate protection • Soft and comfortable • Latex-free • Not as durable • Sensitive to the touch |
| Nitrile gloves | • Protein-free • Latex-free • Allergy-free • Chemical and puncture resistant • Higher level of protection and durability |
2. Latex gloves and allergic reactions
Latex gloves often have a powder coating on the surface which is known to cause skin irritation. It may also cause problems for those with respiratory issues if accidently inhaled. Due to the increasing prevalence of latex allergy, latex gloves are not used in many hospital settings and not recommended. The disposable gloves without powder coating is recommended [6]
3. All perioperative care providers should wear gloves when taking care of patient, especially when they will have physical contact with patient. They are encouraged to use double gloves when handling patient's airway, blood, urine, and other body fluid.
Gowns
Gowns are important personal protective equipment when taking care of patients especially when a contagious disease is suspected or confirmed. Gowns protect the wearer from contracting and spreading of the infectious disease from liquid and solid material. To wear gowns is a critical part of the infectious disease-control strategy [7].
1. Types of gowns for personal protection (Table 3)
Table 3: Types of protective gowns for personal protection [7]. View Table 3
2. What type of gown you should wear?
Perioperative care providers should wear what kind of gowns is based on the risk level, which was set by FDA in 2004, as shown in Table 4. For the protection of perioperative care providers against the infection of COVID-19, the coverall gown which prevents airborne pathogens should be the best in our opinion, because the COVID-19 can be transmitted via normal breathing, coughing, sneezing, surface contact and aerosol/aerated solids or liquid. The correct gown wearing is shown in Figure 2.
Table 4: Risk levels for health care operation [7].
| Risk level | Description | |
| I | Minimal risk | Basic care, cover gown for visitors, standard isolation, or in a standard medical unit |
| II | Low risk | Blood draw, suturing, in the ICU, or a pathology laboratory |
| III | Moderate risk | Arterial blood sampling, inserting an intravenous line, in the Emergency Room, or for trauma patients |
| IV | High risk | Fluid/blood intense procedures, surgery, when pathogen resistance or infectious diseases are suspected (non-airborne) |

Figure 2: Coverall gowns.
Face shield
Face shield has some protective effects against airborne transmission, but it does not offer complete protection. So, for the care of patients with COVID-19, face shield does not have the important role as coverall gown or N95 face mask.
Eye protection
Eye goggles are useful for the protection of eyes, but it does not have the protective effects as face mask does. It is less beneficial in managing patients with COVID-19 when comparing with face mask and coverall gown.
Avoidance of Cross Infection of Respiratory Disease
It is critical to avoid transmission of pathogen between patient and health care providers, and transmission from patient to patient. All measures need to be taken to prevent these cross-infections in the operating room and other perioperative settings.
Anesthesia ventilation system and anesthesia machine
In the United States, all ventilation circuits, humidifiers, and nebulizers used during general anesthesia are disposable and discarded after single use. However, the CO2 absorbent is not routinely replaced after each case. And anesthesia machine is not routinely cleaned or disinfected after each use. Do we need to clean and disinfect the anesthesia machine per se? Especially when we use the anesthesia machine for patients with respiratory infectious disease as the COVID-19 infection? The answer is probably not as long as the breathing system filter (BSF) is used and the BSF has adequate retention efficiency for airborne pathogen. Heuer, et al. tested three BSF models: Pall Ultipor 25, Pall Ultipor 100, and Pall BB50T with initial H1N1 virus load of 7.74 ± 0.27 log10. It decreased a viral load of ≤ 2.43 log10 after the filter, indicating a viral filtration efficiency nearly 100%. Thus, the authors concluded that all three tested filters retained the virus input very well. The use of BSF in the closed ventilator systems for intubated and mechanically ventilated patients could reduce the risk of spreading the virus to the ventilation system and the ambient air. However, in some countries where ventilator circuit is not affordable to be changed routinely after each use, we strongly recommend they must change at least the BSF after each patient. Also, worth noting, the retention efficacy of BSF for liquids is recommended to be at pressures of at least 60 hPa (about 60 cm H2O) or 20 hPa (about 20 cm H2O) above the selected maximum airway pressure in the ventilator system [8,9]. The ventilator can be used for up to 7 days if the functional parameters remain adequate or based on the manufacturer's instructions [8]. The breathing circuit and the manual bag should be immediately changed after each patient care if the following situation has occurred or is suspected to have occurred: Notifiable and/or identifiable infectious disease involving the risk of transmission through the ventilation system and the manual bag, such as tuberculosis, influenza virus, acute viral hepatitis, measles, colonization and/or infection with a multiple resistant pathogen, upper or lower respiratory tract infections including coronavirus infection.
The position of BSF is also important. Protection of the anesthesia machine from the patient would suggest BSF be placed in the expiratory limb, while protecting the patient from the anesthesia machine suggests BSF on the inspiratory limb of the breathing circuit. BSF between the endotracheal tube and the Y-piece would protect both patient and anesthesia machine from contamination and probably makes the most logical sense [10].
If contamination to the ventilatory circuit by blood or other secretions is grossly visible, it is required that the BSF, the anesthesia circuit and CO2 absorbent cannister are all changed and the ventilation conducting parts of the anesthesia ventilator should be hygienically processed [8]. All surfaces of the anesthesia equipment and cart exposed to hand contact must be disinfected after each case. All used supplies should be disposed if all possible.
Hand hygiene
Hand-mediated transmission is believed to be the major contributing factor to the healthcare provider-contracted infections. Hand hygiene is highly recommended be performed according to the World Health Organization guidelines [11]. Hand Hygiene should be performed before all aseptic tasks. The anesthesia providers are encouraged to consider using double gloves during airway manipulations, with removal of the outer gloves immediately after intubation. In addition, the placement of alcohol-based hand rub dispensers was recommended at the entrances to the operating rooms and near anesthesia providers. These providers should also change gloves and perform hand hygiene between doffing and donning infection prevention equipment.
Airborne precautions
Airborne precautions are used to prevent transmission of infectious agents that remain contagious when suspended in the air (COVID-19, M. tuberculosis, varicella virus [chickenpox], influenza virus, and rubeola virus [measles], Severe Acute Respiratory Syndrome (SARS)-CoV etc.). A respiratory protection educational program should be implemented. This includes education of respirator use, fit testing, and user seal checks followed by a knowledge test to ensure proper mastery of the airborne precautions. In perioperative settings, all patients should wear a face mask of N95 or higher-level respirator. After induction of general anesthesia and endotracheal intubation, patient's endotracheal tube should be connected to a circuit with disease specific BSF if possible. After surgery is done, the patient should be either discharged to the home environment or transferred to a facility with an airborne infection isolation room. If possible, individuals who are not vaccinated should not care for patients with vaccine-preventable airborne diseases (measles, chickenpox, and smallpox). After surgery is completed and patient is transported out of the operating room, the operating room should not be used immediately for another surgical procedure. These patients should go to the operating room directly to bypass pre-anesthesia holding area in attempt to minimize transmission to other patients or healthcare providers. If this not possible, a separate isolation room for the patient should be available [12].
Droplet precautions
Droplet precautions are aimed to prevent transmission of pathogens (like flu, COVID-19 etc.) from the lungs and upper airways (nose, mouth, throat etc.) These pathogens can spread via respiratory and mucous membrane contact. These pathogens generally do not remain infectious over long time and over relatively long range in health care facilities. However, it seems that COVID-19 could potentially survive much longer time in the air than previously believed. Droplet Precautions are indicated including COVID-19, influenza virus, flu virus, adenovirus, SARS, pertussis, rhinovirus, meningitides, and group A streptococcus (for the first 24 hours of antibiotics therapy). A single room is preferred for the patient who requires droplet precautions. More than 3 feet spatial separation and having a curtain between patient beds are also recommended in a room with multiple beds. Healthcare personnel should wear a mask (a respirator is not absolutely necessary) when taking care of patients with droplet precautions with close contact.
If a patient on droplet precautions need to be transported outside of the room, the patient should wear a mask if patient tolerates, and follow respiratory hygiene/cough guideline. In the preoperative holding area, a separate isolation room for the patient should be prepared and readily available for a patient who is on droplet precautions [12].
Special Considerations in Perioperative Care
A. Individual identification
Since all perioperative care providers are covered by the coverall gowns, it is very difficult to identify each individual, thus it is important to label each individual's name on their gown or cap to facilitate the communication among healthcare providers, as shown in Figure 3.
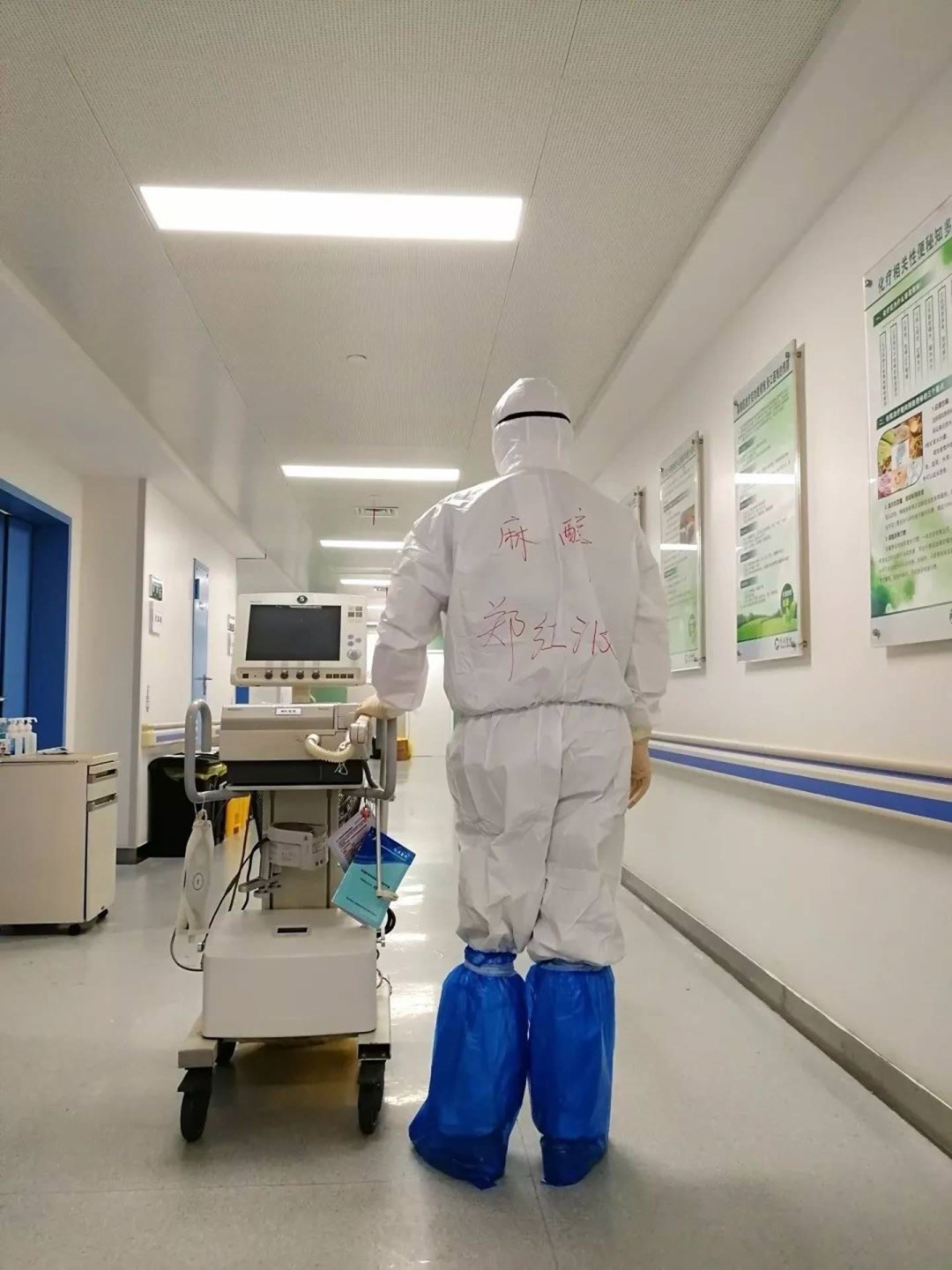
Figure 3: Department (Anesthesiology) and provider's name (Hongbo Zheng) are written on the gown. This photo is retrieved from the public news report [13].
B. Medication identification and verification
When physicians and nurses are in the coverall gowns, the hood does not provider great transparency and visibility, it is critical for perioperative care providers to ascertain the name of the medication is exactly what they intend to administer to the patient.
C. Endotracheal intubation and confirmation of tube location
When anesthesia provider intubates a patient and place an endotracheal tube, in addition to double glove and minimize the chance to traumatize themselves, the poor visibility through the hood will make intubation process much harder and it is very difficult to confirm the breath sound by auscultation, as shown in Figure 4. End-tidal CO2 and chest rise are the best indications of correct endotracheal intubation. As soon as endotracheal tube is in, the outside layer of gloves should be removed immediately. Regarding ventilatory settings, we would recommend using lower tidal volume, lower airway pressure and higher frequency ventilation. It is recommended to use disposable intubating equipment.

Figure 4: Intubation while wearing a coverall gown.
D. Verbal communication
In an environment with all the providers are inside the gowns, verbal communication could be a huge issue, voice is baffled, and hearing is decreased. Speakers need to talk significantly louder to ensure clear communication for patient safety, and additional body language will need to be used.
E. Room temperature setting
Since all personnel in the operating room are wearing multiple layers of clothing, feeling hot and sweating can very likely be a problem, especially for the surgeons. Adjustments to the room temperature setting needs to be made before surgery starts. If in other disaster scenarios like earthquake, hurricane, electricity and air-conditioning become unavailable, this can truly be a major problem, especially in the South and in the summer time (Figure 5).
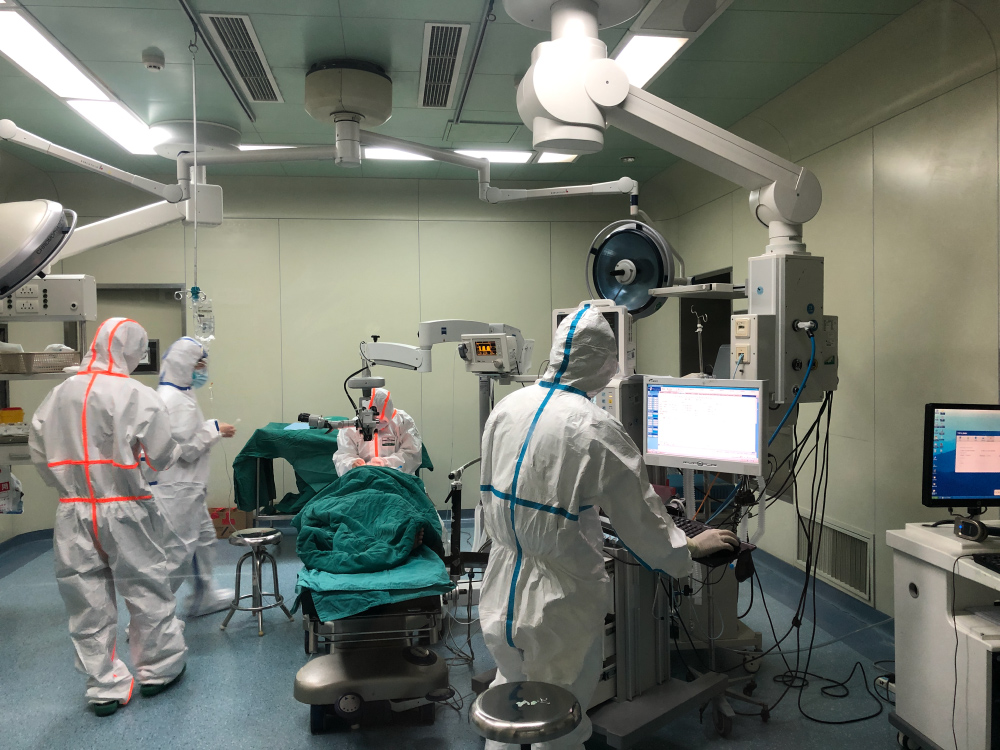
Figure 5: An example of operating room environment in preventing cross-infection for airborne infectious disease.
F. Discussion with patient and obtaining informed consent
This can be challenging process also. The communication between medical team and patient is a process of face-to-face communication involving facial expression and emotional gestures, now both patient and physicians wearing face mask or gowns, barely see each other's faces and emotion, the communication process won't be as effective as normally we have. Obtaining an informed consent can be difficult because the hard copy consent and the signing pen per se can be a carrier of pathogen, using digital/video consent and witness may be the alternative.
Establishment of Anesthesia Departmental Protocol for Patient with Respiratory Infectious Disease
We recommend the protocol include the following:
A. Identify the risk level of a patient with respiratory infectious disease, alert pertinent healthcare personnel. An infectious control leadership team should be established as part of the disaster preparation team.
B. Precautions against the transmission of infection among patients and perioperative care providers should be a routine part of perioperative patient care.
C. When the patient needs transportation, the patient should always wear a N95 mask or higher-level respirator. To minimize potential exposure and easy decontamination, special transportation route should be well planned as suggested in one of the recently published papers [14].
D. Surgical patient with respiratory infectious disease should be scheduled to go to the operating room directly bypassing paranesthesia holding area. If this is not possible, a separate isolation room should be available for this kind of patient.
E. Hand hygiene should become a culture for all perioperative care providers who should always wear appropriate gloves. It is recommended to wear double gloves when handling airway, blood, urine and any other body fluid. Gloves should be changed after each procedure and between different patients, and gloves must be disposed as infectious waste, and hands must be washed with soap and water or decontaminated after removing gloves.
F. Specifically, for patient with COVID-19, a coverall protective gown with hood is recommended but not absolutely required (authors' opinion and recommendation).
G. If not wearing a coverall protective gown, perioperative care providers should wear a N95 mask or higher-level respirator, ensuring there is no gap between mask and the face. Using a tape to seal the perimeter of the mask is also recommended.
H. Shoes or other footwear should be worn in the procedure suites and covered with shoe covers.
I. All anesthesia related equipment and surface should be cleaned and decontaminated before and after each surgical procedure, especially so when taking care of patient with respiratory infectious diseases.
J. Appropriate antibiotics should be administered based on bacterial culture result and/or surgical procedure.
K. After surgery, all ventilatory circuit and filter should be disposed and replaced.
L. All routine universal precautions should be applied, as needle precaution, intravenous fluid, drug and syringe.
M. If patient with respiratory infectious disease needs bronchoscopy, the bronchoscope needs to be sterilized after use.
N. All perioperative service departments should have a team which conducts crisis management simulation for the whole department.
Summary
Significant challenges exist for perioperative care providers when caring for patients with the COVID-19 in ICU or perioperative settings. Adequate personal protection and avoidance or minimization of cross-infection cannot be over-emphasized. We summarized the preventive measures of cross-infection, recommending isolation room in paranesthesia holding area or straight to the operating room bypassing paranesthesia holding area, ventilation circuit filter use, circuit and BSF replacement after each use, airborne and droplet precautions, and establishing department and hospital-wide protocols for management of patients with respiratory infectious diseases. Many unexpected difficulties such as poor visibility inside the coverall gowns, difficult to communicate verbally due to voice baffling, providers may become hyperthermia and sweating inside the gowns, difficult to communicate with surgical patient and obtaining informed consent, will be encountered by perioperative care providers. Since many aspects regarding COVID-19 are evolving, our management strategy is preliminary, and changes will be needed in the future.
References
- Li Q, Guan X, Wu P, Wang X, Zhou L, Tong Y, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus–infected pneumonia. N Engl J Med. 2020 Jan 29. doi: 10.1056/NEJMoa2001316. DOI: 10.1056/NEJMoa2001316
- Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, et al. Clinical Characteristics of 138 Hospitalized Patients With 2019 Novel Coronavirus–Infected Pneumonia in Wuhan, China. JAMA. Published online February 7, 2020. doi:10.1001/jama.2020.1585
- Lu C, Liu X, Jia Z. 2019-nCoV transmission through the ocular surface must not be ignored. The Lancet. Published: February 06, 2020, DOI:https://doi.org/10.1016/S0140-6736(20)30313-5
- https://zhuanlan.zhihu.com/p/48521349 (Last accessed on February 9, 2020)
- https://www.who.int/emergencies/diseases/novel-coronavirus-2019/advice-for-public/when-and-how-to-use-masks (Last accessed on February 9, 2020)
- https://bulknitrilegloves.com/types-of-medical-gloves-and-their-uses/ (Last accessed on February 9, 2020)
- https://www.fda.gov/medical-devices/personal-protective-equipment-infection-control/medical-gowns#g2 (Last accessed on February 12, 2020)
- Kramer A, Kranabetter R, Rathgeber J, Züchner K, Assadian O, Daeschlein G, et al. Infection prevention during anaesthesia ventilation by the use of breathing system filters (BSF): Joint recommendation by German Society of Hospital Hygiene (DGKH) and German Society for Anaesthesiology and Intensive Care (DGAI). GMS Krankenhhyg Interdiszip. 2010; 5(2): Doc13. Sep 21. doi: 10.3205/dgkh000156.
- Heuer JF, Crozier TA, Howard G, Quintel M. Can breathing circuit filters help prevent the spread of influenza A (H1N1) virus from intubated patients? GMS Hyg Infect Control. 2013 Apr 29;8(1):Doc09. doi: 10.3205/dgkh000209
- Krueger P, Klos C, Paulsen AW, Klauss G, Blessing R, Kimatian S, et al. Cross-aontamination via anesthesia equipment? APSF Newsletter. 2009. 24 (1): 1-24
- Gemmell L, Birks R, Radford P, Jeffries D, Ridgway G, McIvor D. Infection control in anaesthesia. Anaesthesia. 2008 Sep;63(9):1027-36. DOI: 10.1111/j.1365-2044.2008.05657.x
- Siegel JD, Rhinehart E, Jackson M, Chiarello L, The Healthcare Infection Control Practices Advisory Committee. Preventing transmission of infectious agents in healthcare settings. http://www.cdc.gov/ncidod/dhqp/pdf/isolation2007.pdf (Last accessed on February 12, 2020)
- https://mp.weixin.qq.com/s/1Cjo8-CvIU8OeVp6NNVnzw (Last accessed on February 12, 2020)
- Park J, Yoo SY, Ko JH, Lee SM, Chung YJ, Lee JH, et al. Infection Prevention Measures for Surgical Procedures during a Middle East Respiratory Syndrome Outbreak in a Tertiary Care Hospital in South Korea. Sci Rep. 2020 10(1):325